Transperineal Prostate Biopsy
On average, I think men tend to be somewhat “mystified” when it comes to PSA testing and perhaps more so when it comes to the significance of test measurements. Many believe a PSA test, or more properly a prostate-specific antigen test, is designed to find cancer. It is not.
Yet for many men, just knowing they may receive a possible cancer diagnosis is enough to have them avoid MD visits and, in the process, miss out on the opportunity to get a simple blood test.
PSA versus biopsy
PSA is a protein which is produced by both normal and malignant cells in the prostate gland. The blood test only measures the level of the protein in a man's blood. A prostate biopsy is quite different and offers a way to identify if you have prostate cancer. Being referred for a biopsy generally can mean that your doctor suspects that you may have cancer.
A steady rising PSA, along with detecting some irregularities during a digital exam of the prostate, is often enough to refer a patient to a urologist. Other indicators can also trigger the need for a biopsy.
The biopsy process
A common type of biopsy uses a fine needle attached to a finger-sized probe which is inserted into the rectum. Once in place, it is guided to various target areas using ultrasound images.
A more advanced system incorporates the use of MRI images or magnetic resonance imaging.1 Both methods fire a fine needle through the rectal wall to gather prostate tissue. The samples are then sent to a pathologist, who assigns an aggressiveness score. An issue with biopsies is that the sampling needle passes through the rectal wall, and in the process may carry bacteria into your blood stream and cause an infection. Modern antibiotics can help address the concern.
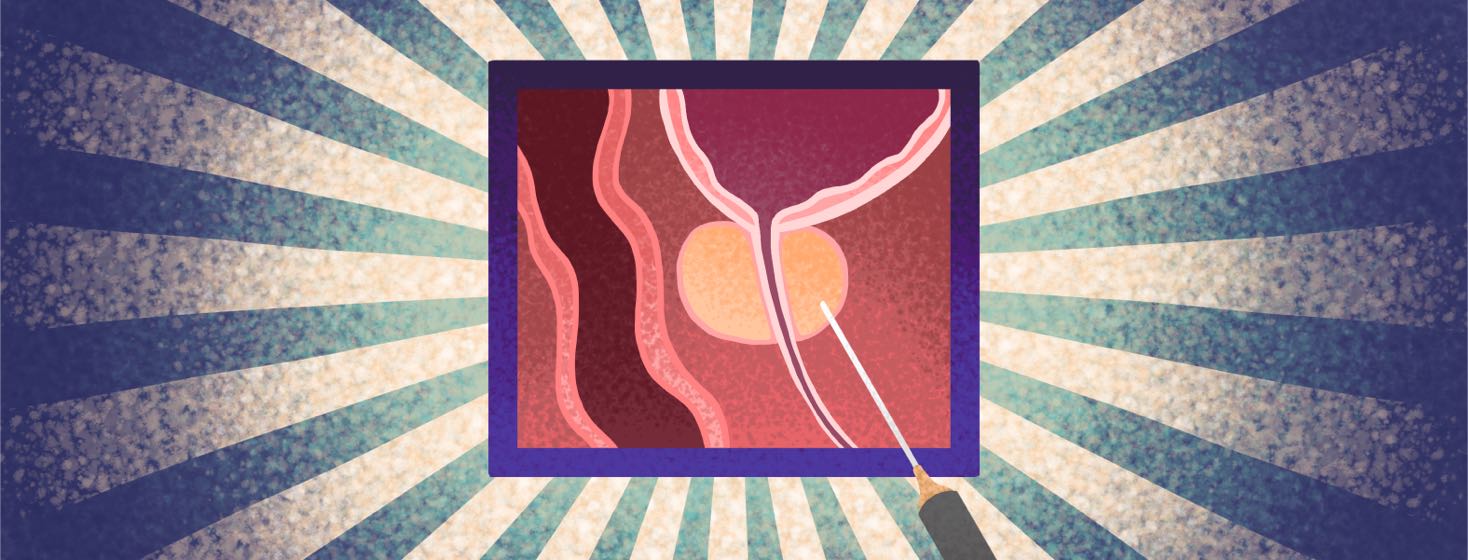
The transperineal approach
A newer and more accurate approach is called “transperineal,” and it eliminates the need to put a biopsy needle through the rectal wall. Sampling is done by passing a needle through the region between the scrotum and the anal opening. An advantage of this system is that it reduces the possible danger of an infection. A second benefit is it allows the urologist to examine and biopsy the back side of the prostate (the anterior zone), where aggressive cancers can be missed.2,3
While this biopsy method is newer and not as commonly utilized by urologists, patients who have undergone the procedure report that discomfort following the test can be managed with over-the-counter pain medications. Another side effect of the procedure could be temporary bruising where the needle was entered.4
Potential of blood in semen
With any prostate biopsy, men may have blood in their semen for days or several weeks. After my own biopsy, I was a bit shocked to see how much blood was present in a discharge. During this time men may also experience some loss of interest in sexual activity.
Today if you are scheduled for a biopsy, I think it could be good to ask your urologist if they are using the transperineal method. Whichever you choose, I think a biopsy – not a PSA test – is the best way to know if you are facing prostate cancer.
Join the conversation