Coping with Side Effects of Prostate Cancer Treatment
Reviewed by: HU Medical Review Board | Last reviewed: March 2026 | Last updated: April 2026
Prostate cancer is a common health condition in men. Many cases of prostate cancer can be successfully managed. However, the potential long-term side effects of these treatments can be hard to manage in some cases.1
Every treatment option has a different set of potential side effects. Some side effects happen right away. Others may appear months or years after treatment ends. It is important to know what to expect. This knowledge helps you and your caregivers prepare for the journey ahead.1
What are the possible treatment side effects?
Prostate cancer treatment options include surgery, radiation, and medications, such as hormone therapy. Each one impacts the body in different ways. If you are worried about a specific side effect, talk to your doctor. They may be able to suggest a treatment with a lower risk for that issue.1
Common side effects include bowel problems, hot flashes, lymphedema, and incontinence. These issues can affect your daily life and your mood. Your healthcare team is there to help you manage these changes. You should always report new symptoms to your medical team as soon as they appear. Early intervention often leads to better results.1
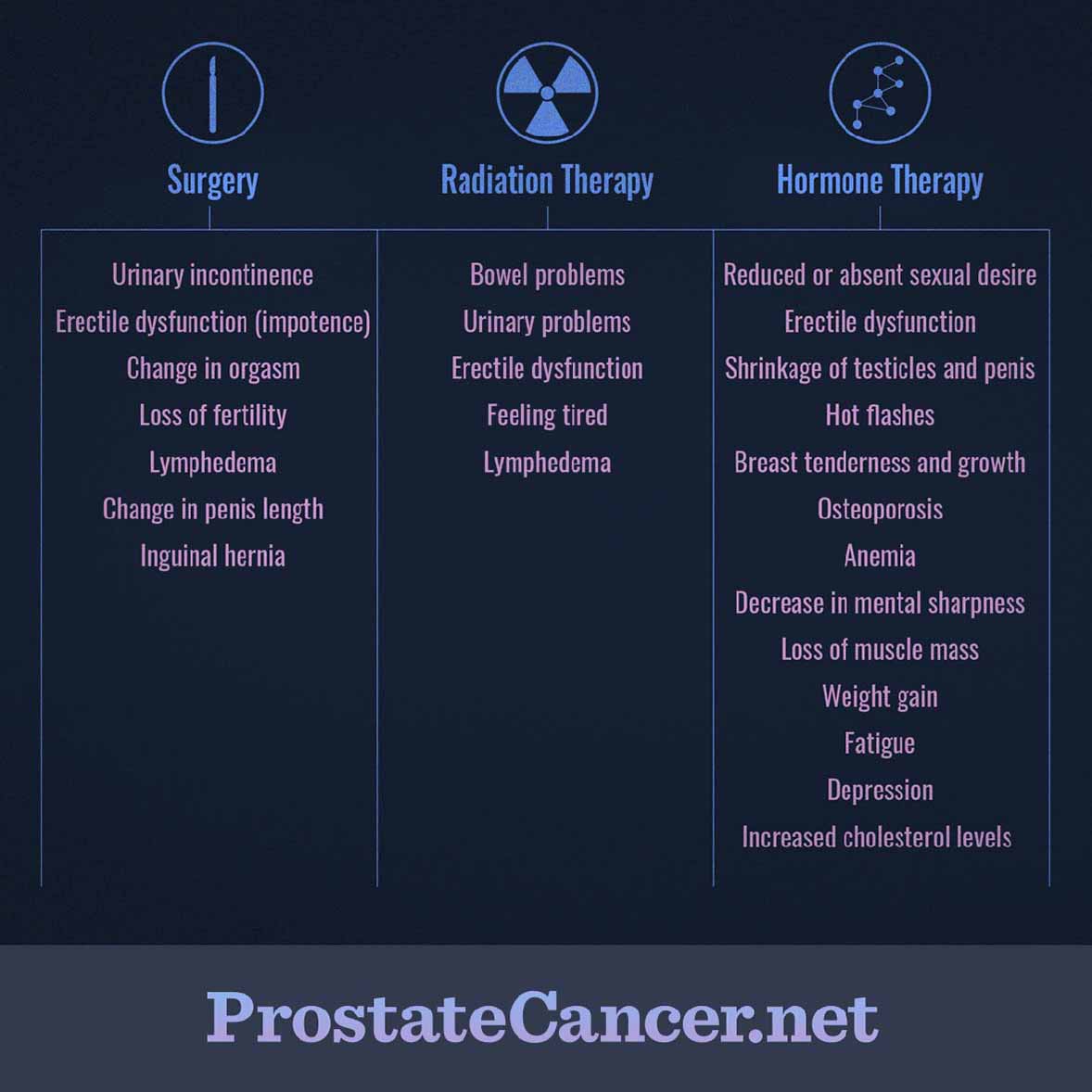
Common side effects of treatment that can impact your quality of life are listed by treatment type in the table below:
Figure 1. Side effects of primary treatment options
This is not an exhaustive list of all potential treatment-related side effects that can impact quality of life. If you’re experiencing something not on this list that is impairing your overall wellbeing, seek medical attention.
Managing bowel problems
Radiation therapy for prostate cancer can sometimes affect the rectum. This is because the rectum sits very close to the prostate gland. When the rectum is irritated, it can cause bowel problems. These problems may include diarrhea, gas, or an urgent need to have a bowel movement. Some people also experience leaking from the bowels. This is called fecal incontinence.1
You can manage these issues in several ways. Your doctor might suggest a low-fiber diet for a short time to rest your system. Drinking plenty of water is also very important (check with your doctor if you have a fluid restriction). Some people find relief by using over-the-counter medications.1
Check with your doctor before taking any new medicine. Pelvic floor exercises can also strengthen the muscles that control bowel movements.1
Understanding hot flashes
Hot flashes are often linked to hormone therapy. This treatment lowers the level of testosterone in the body. When testosterone levels drop, the body has trouble controlling its temperature. A hot flash feels like a sudden wave of heat. It usually starts in the face or chest and spreads through the body. It may cause sweating or a fast heartbeat.1
You can cope with hot flashes by making small changes. Wear loose clothing made of natural fibers like cotton. Keep your home cool with fans or air conditioning. Some people find that spicy foods, caffeine, or alcohol make hot flashes worse. Avoiding these triggers may help. In some cases, doctors prescribe medications to reduce the frequency of hot flashes.1
Dealing with lymphedema
Lymphedema is a type of swelling that occurs when lymph fluid cannot drain properly. This often occurs if lymph nodes were removed during surgery, or damaged by radiation, in a certain part of the body. The swelling can cause a feeling of heaviness or tightness in the skin. It can also make it harder to move your legs if the lower body is affected.2
Managing lymphedema requires careful attention. Compression garments can help move fluid out of the affected area. Special types of massage, called manual lymph drainage, are also helpful. You should try to avoid skin injuries in the areas that are swollen. Infections can make lymphedema much worse. Regular, gentle exercise is also recommended to keep the fluid moving.2 Follow your doctor’s instructions about how to best manage lymphedema in your specific case.
Addressing urinary incontinence
Urinary incontinence is the loss of bladder control. It is a very common side effect after prostate surgery or radiation. You may leak urine when you sneeze, cough, or lift something heavy. This is known as stress incontinence. Some people feel a sudden, strong urge to go and cannot reach the bathroom in time.1
There are many ways to treat incontinence. Pelvic floor muscle exercises, or Kegels, are very effective. These exercises strengthen the muscles that hold back urine. You can also try bladder training. This involves going to the bathroom on a set schedule.1
If these methods do not work, check with your doctor, as they may suggest medications or a small surgical procedure. Using pads or protective underwear can also give you more confidence when you are out in public.1
Mental and emotional support
Dealing with physical side effects can be a heavy burden. It is normal to feel sad, frustrated, or anxious. You do not have to face these feelings alone. Talking to your spouse, partner, or friends can provide great relief. Open communication helps your loved ones understand how to support you best.3
Your healthcare team can refer you to a mental health professional. Counselors and therapists can teach you coping skills for stress. Support groups are another great resource. These groups connect you with other people who are going through the same thing. They can offer practical tips and emotional comfort. Taking care of your mind is just as important as taking care of your body.3